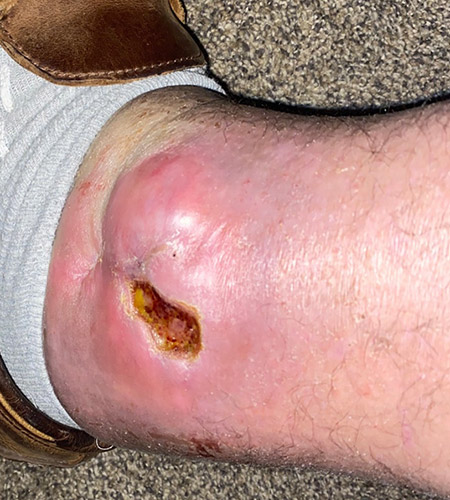
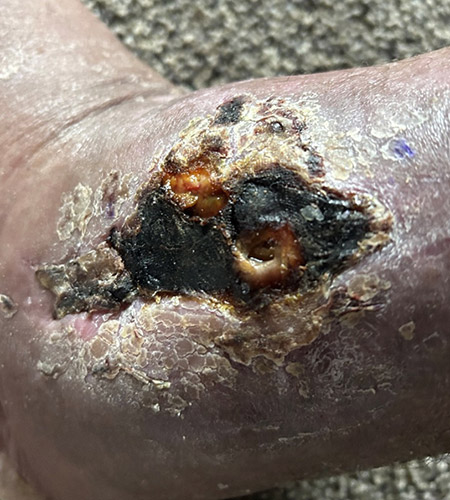
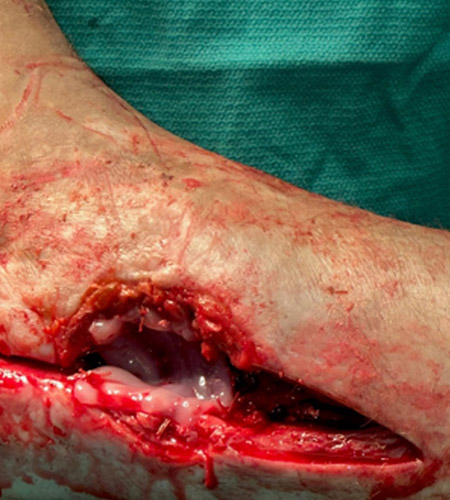
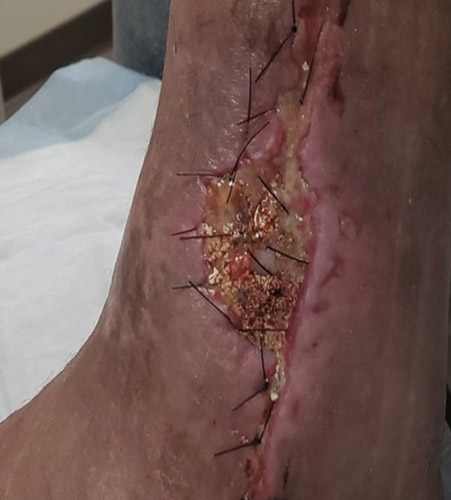
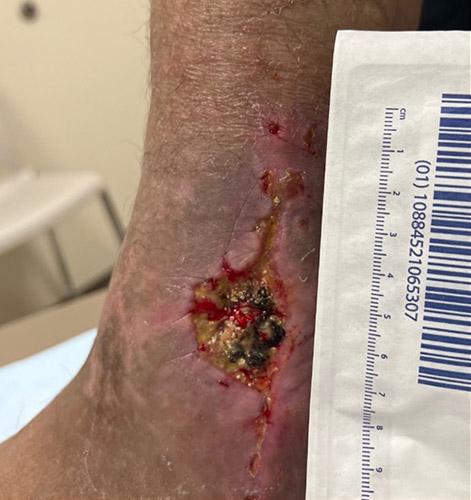
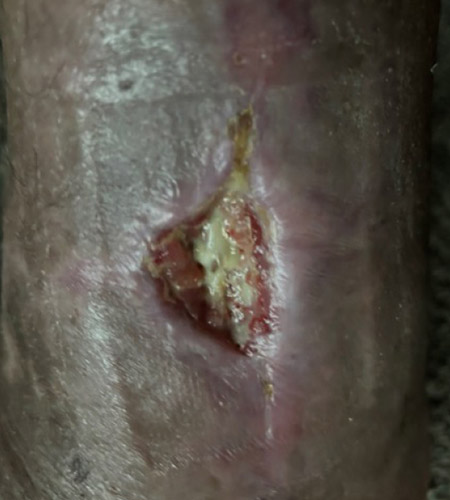
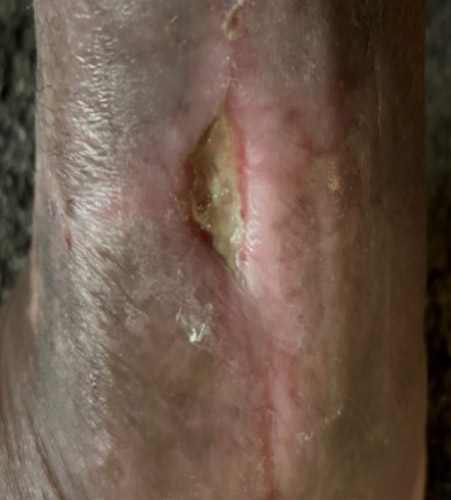
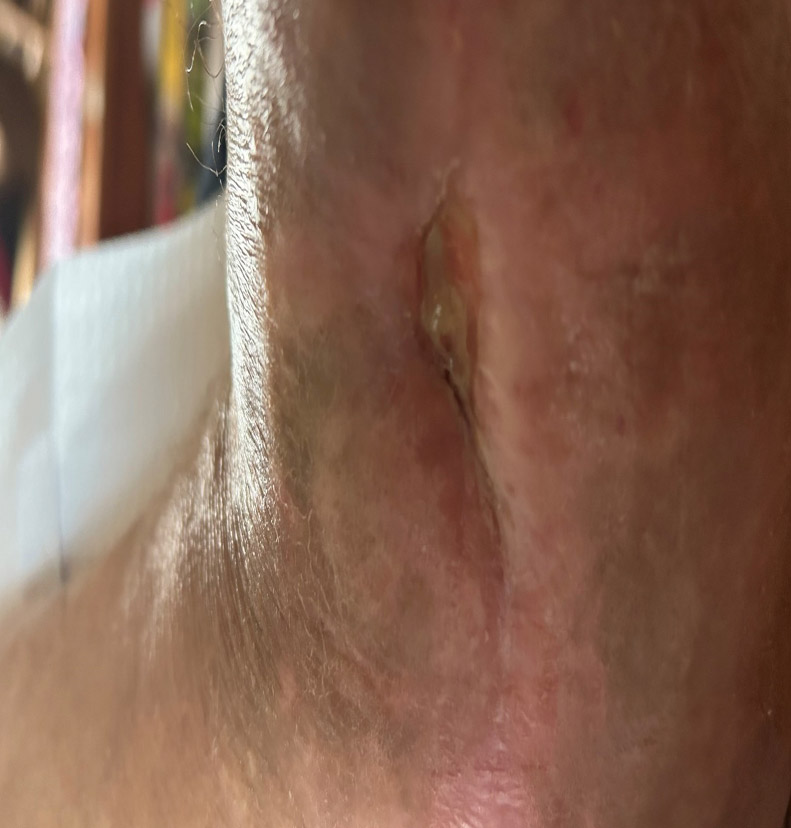
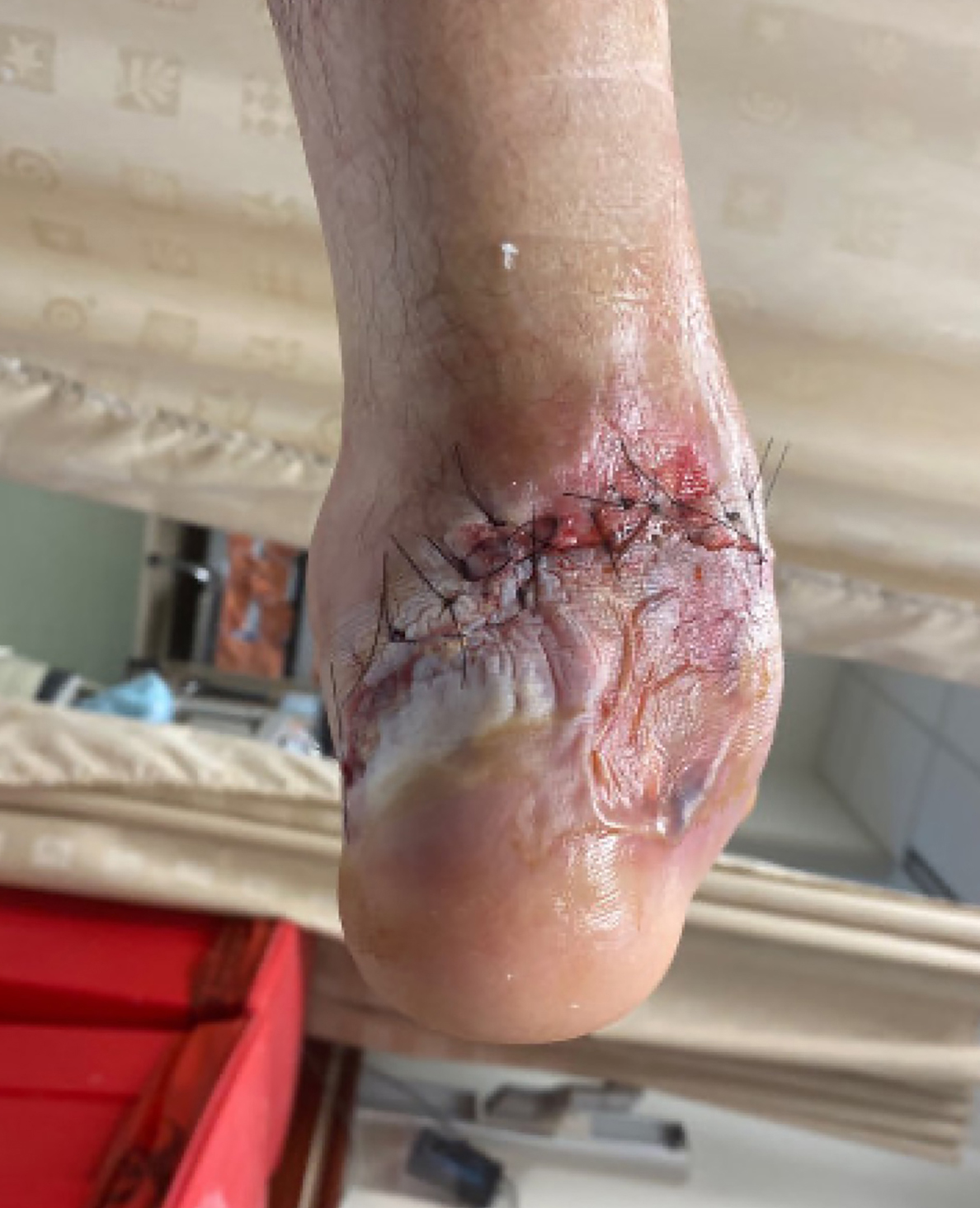
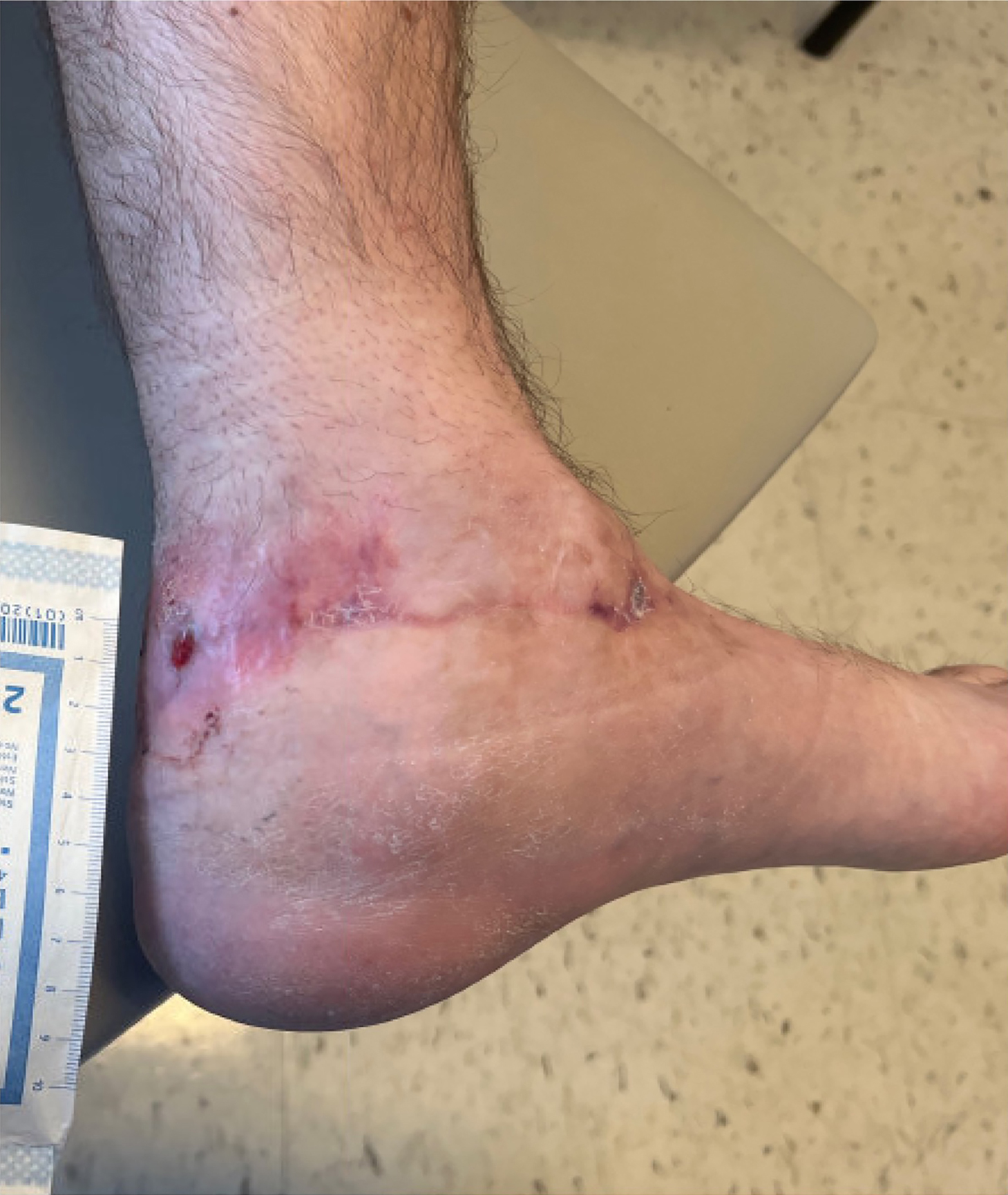
A 57-year-old male with a past medical history of lupus, hypertension, and GERD underwent management for a total ankle replacement complication. The patient had a 3-month-old wound following previous debridement and negative-pressure wound therapy.
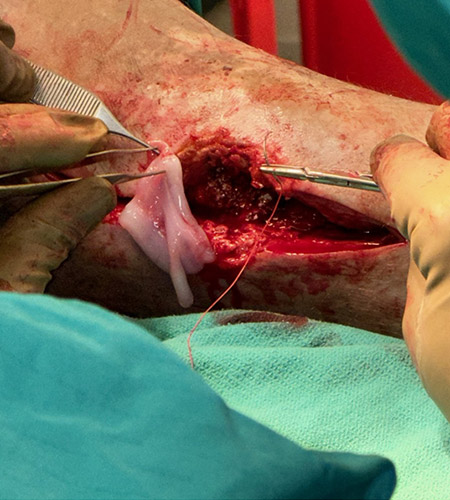
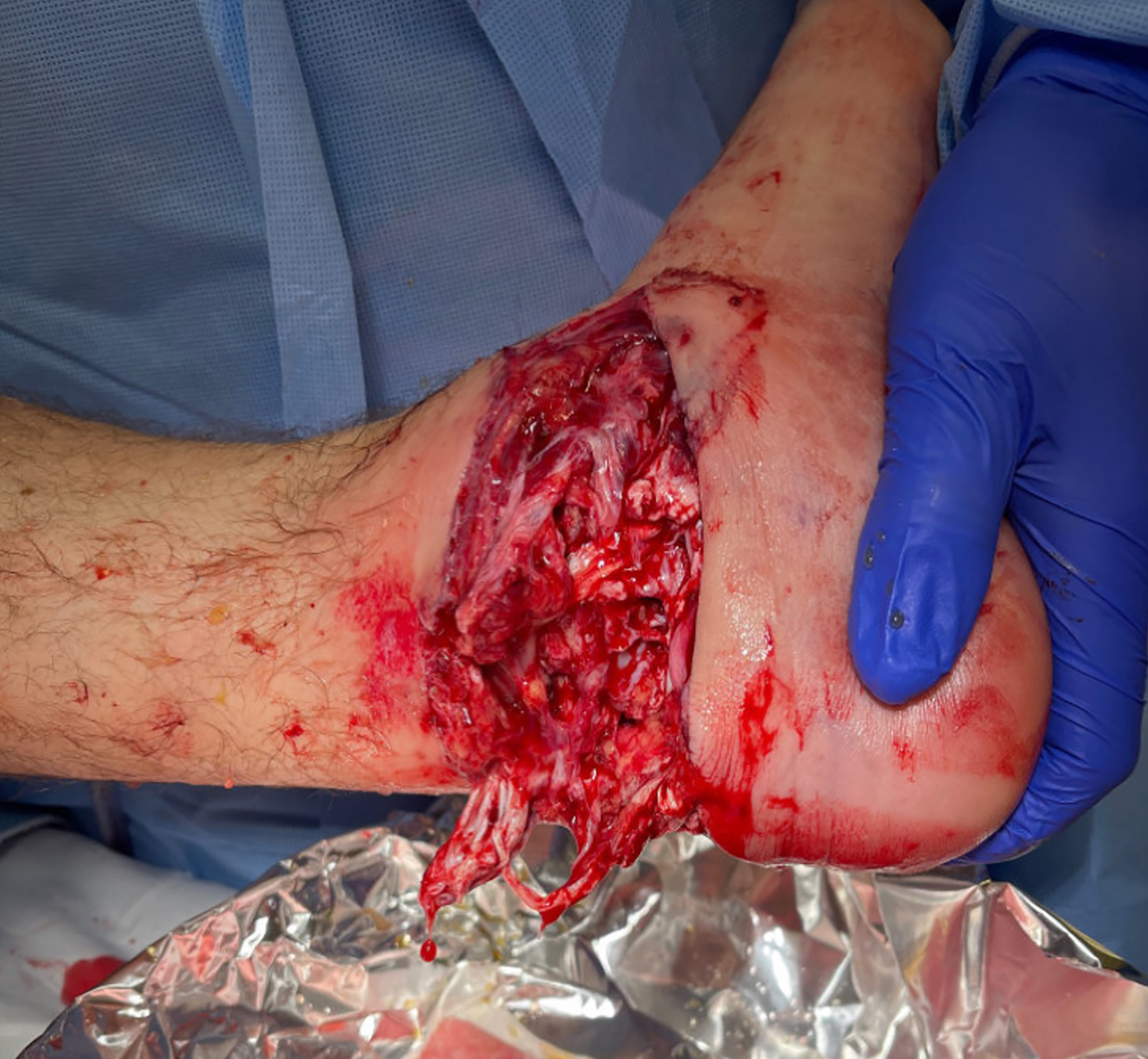
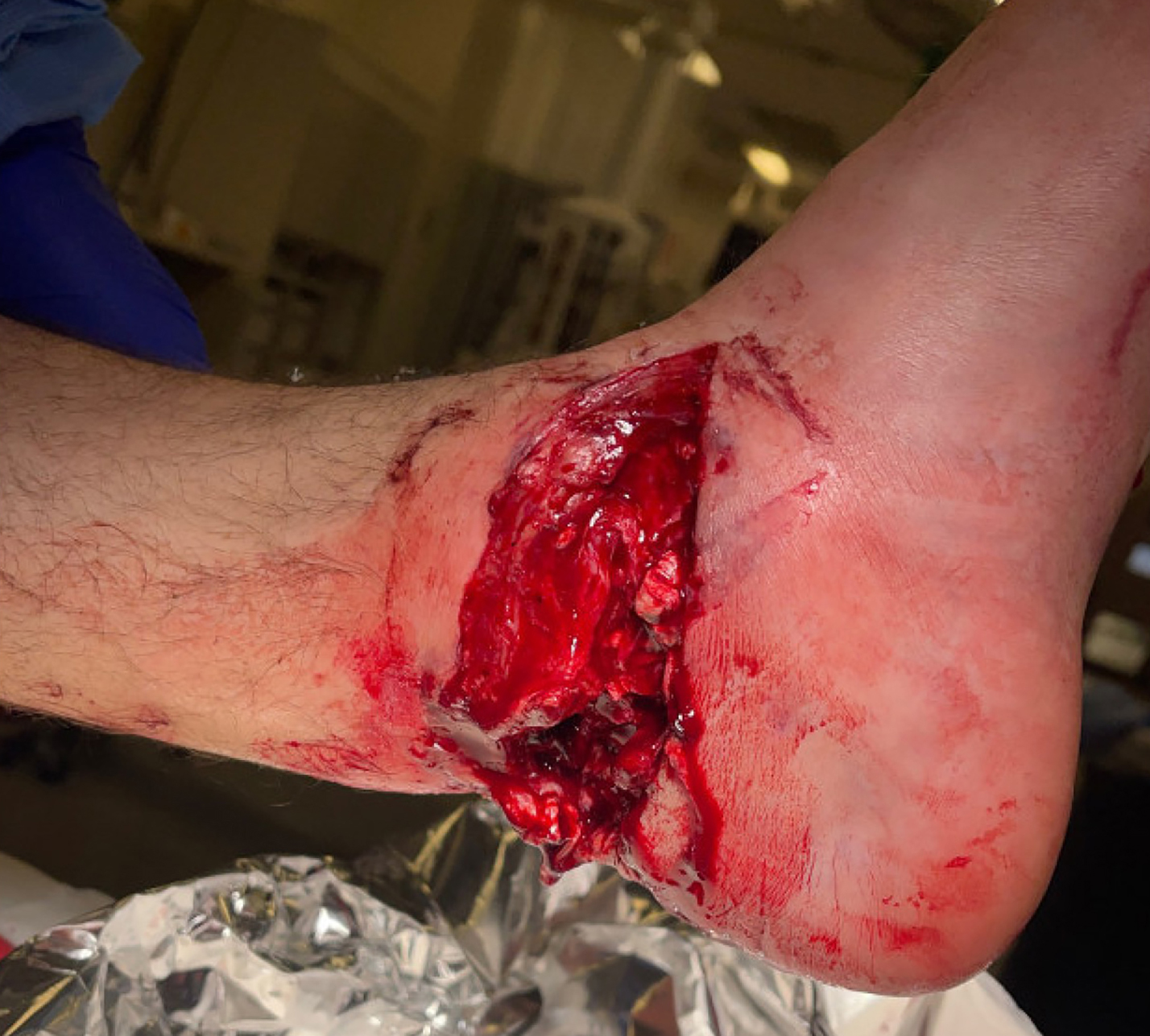
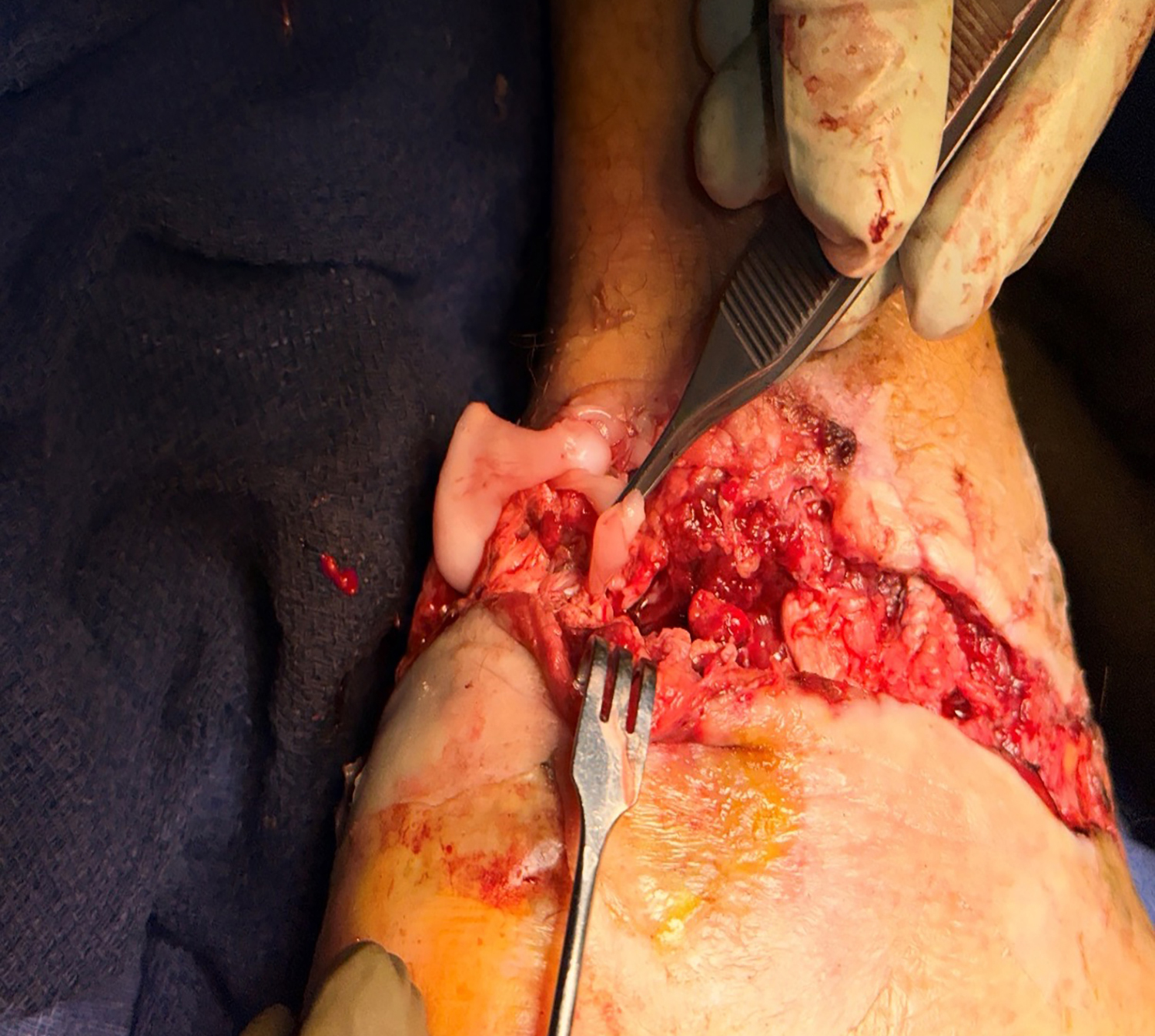
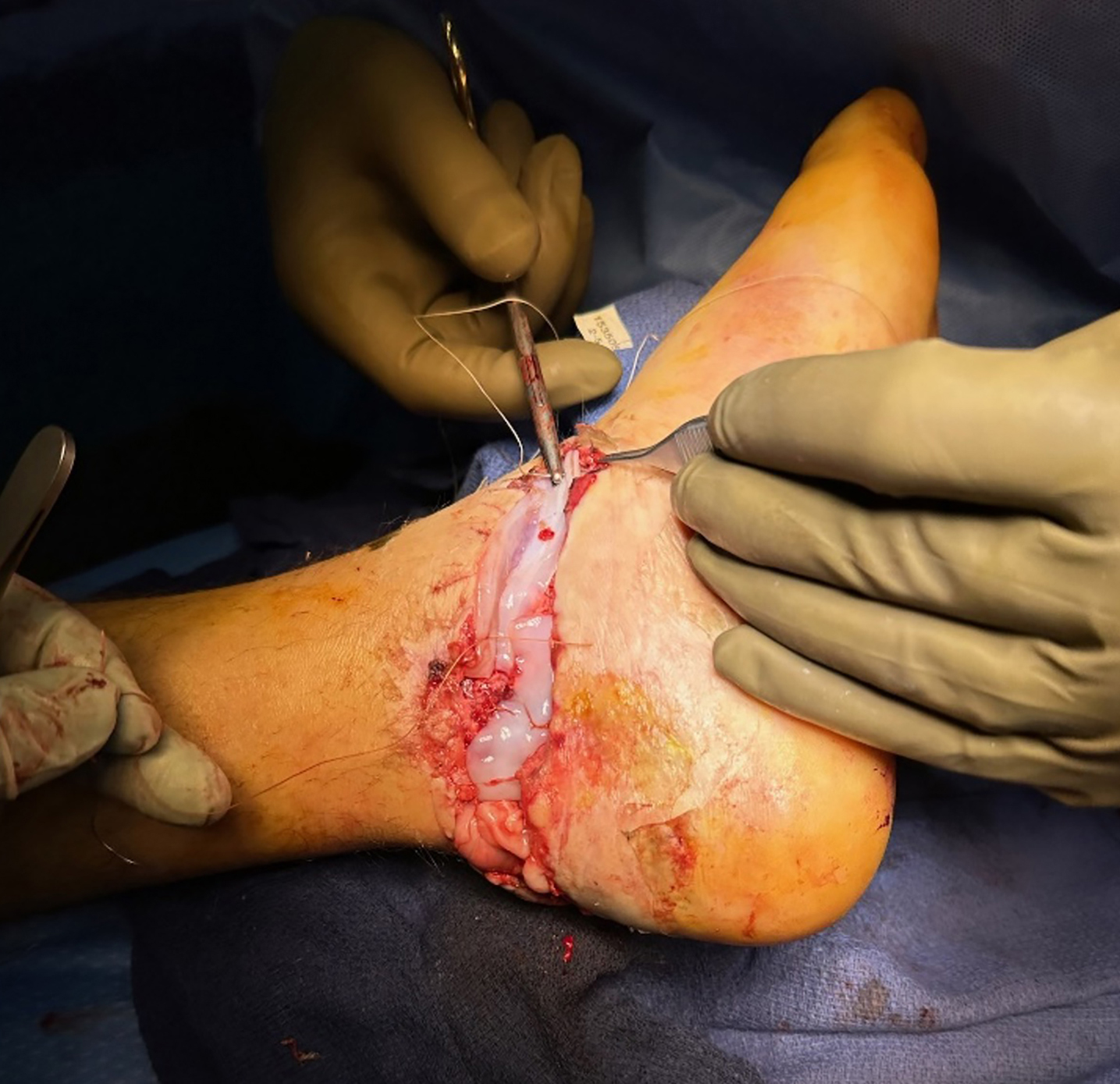
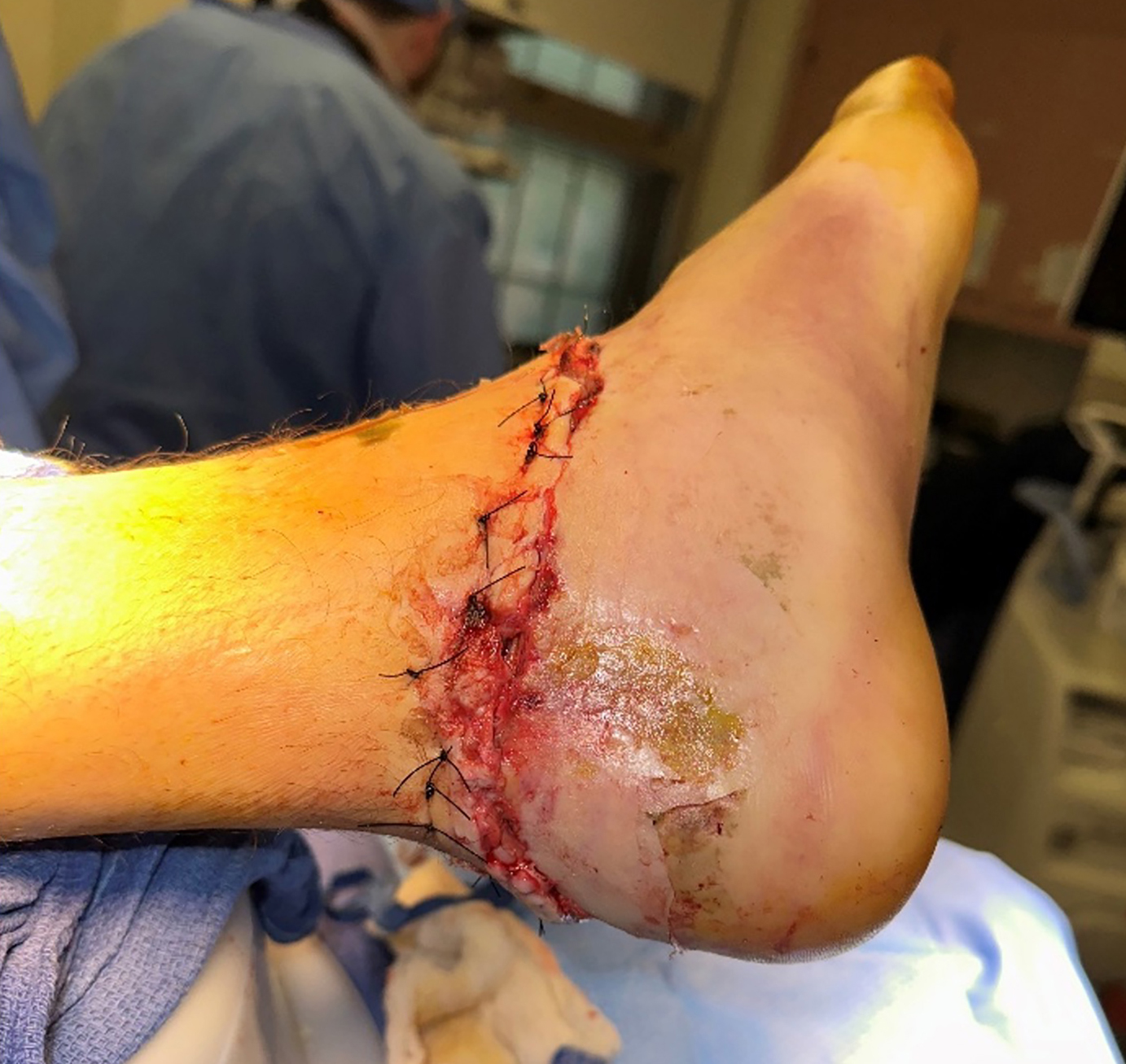
Surgical management involved removal of the total ankle replacement and placement of a cement spacer for six weeks. Following this, a tibiotalocalcaneal (TTC) nail was inserted along with bone grafting to achieve ankle fusion. STRAVIX tissue was applied during the procedure.
Postoperatively, the patient was non–weight bearing for six weeks. Wound care consisted of Xeroform and 4x4 dressings with a splint for the first two weeks. This was followed by casting for two additional two-week periods, with dressing changes at each cast change. After the casting period, the patient transitioned to Xeroform, 4x4’s, Kerlix, Ace wrap, and a CAM boot, allowing weight bearing as tolerated (WBAT).